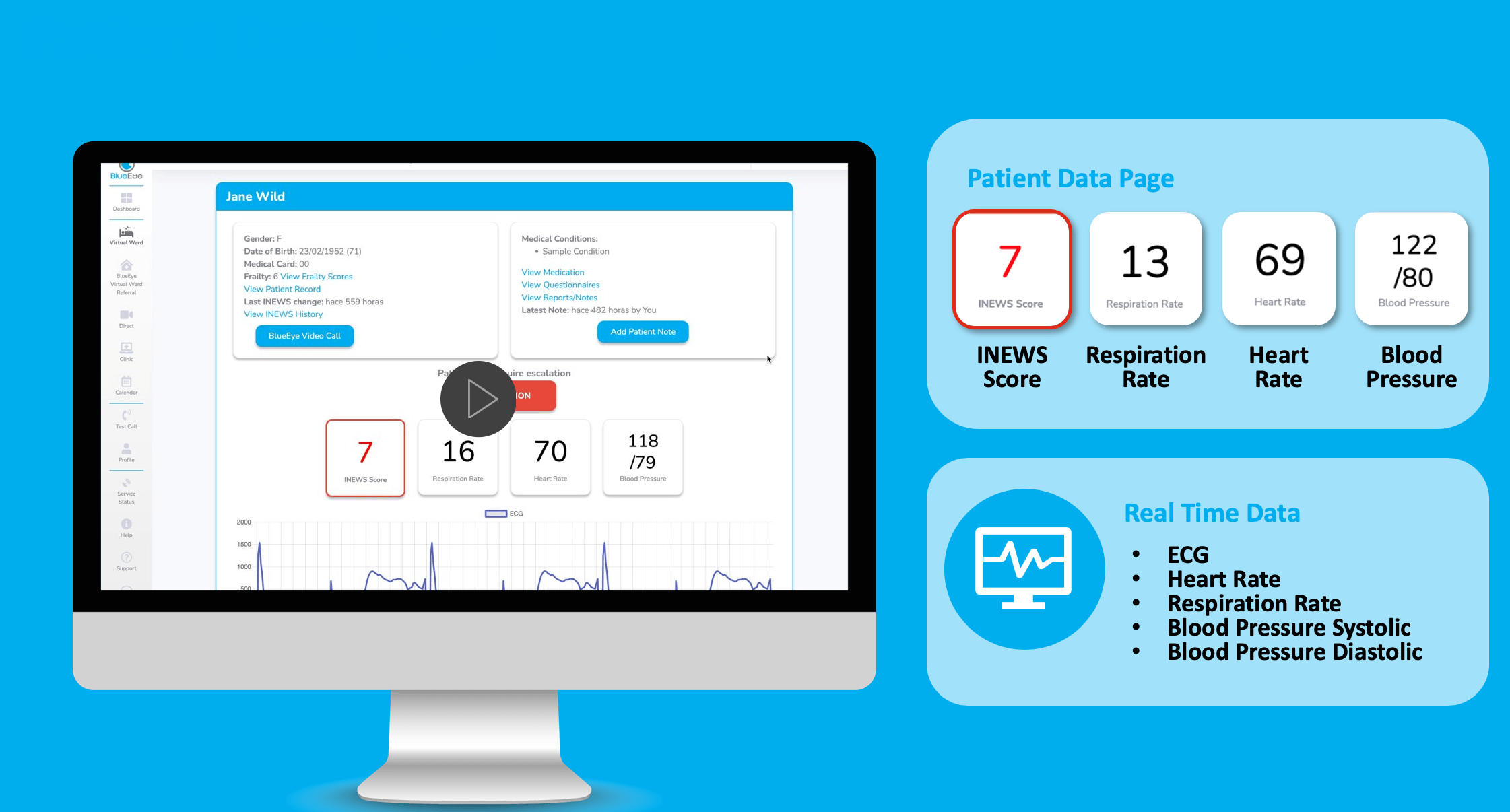
Fig. BlueEye Virtual Ward dashboard showing a patient’s live INEWS score and vital signs readings
Virtual wards are emerging as an innovative solution to provide hospital-level care to patients in the comfort and safety of their own homes. This approach, supported by advanced healthcare monitoring technology, offers numerous benefits such as reducing hospital readmissions, increasing hospital bed availability, optimizing costs, and providing greater comfort for patients. In this article, we will explore the concept of virtual wards and how they are transforming healthcare delivery.
Reducing Hospital Readmissions and Increasing Bed Availability
By monitoring patients remotely after they are discharged from the hospital, virtual wards significantly reduce the likelihood of readmissions. For example, a HSE research study conducted in North Dublin demonstrated an 87% reduction in readmissions to the Emergency Department among older persons (+65 years) using a community virtual ward.
Moreover, there was an 81% reduction in bed days used during the demonstration period.1;2
This reduction in readmissions not only improves patient outcomes but also frees up hospital beds, allowing them to be available for patients who truly need them.
Optimising Costs
In the same HSE study, a comparison was made between the cost of a Community Virtual Ward (CVW) stay and the cost of an Acute Hospital stay, over a twelve-month period.
See table below for costs. These costs were based on an 11 day average stay for approximately 1,980 patients over 3 hospital/community sites. The cost of one patient CVW admission is estimated at €88 per day compared to €820 per day for an acute hospital. The cost of care based on 11-days stay is €969 in a CVW compared to €9,020 in an acute hospital while the cost of care per site is €639,540 for a CVW and €5,953,200 for an acute hospital.
It was estimated that a CVW across three hospital/community sites has the potential to save almost 16 million euros per year in care delivery.
Source: The testing and results of an integrated nurse-led community virtual ward proof-of-concept (page 44). https://assets.gov.ie/138959/f389d9a6-2a32-4c57-aa8d-98f9aa9c8de4.pdf
Implementing virtual ward techniques optimises healthcare costs. Compared to acute hospital admissions or long-term care, delivering care through virtual wards has been found to be 50% more cost-effective. 1;2 By providing access to care at home, virtual wards offer a more efficient alternative to traditional hospital care, reducing the financial burden on healthcare systems.
Reduced risk of hospital based infections
Many individuals are apprehensive about hospitals, particularly during times of pandemic and infection risks. Some patients can pick up infections during a hospital stay which can be avoided through a home hospital stay.
Enhanced patient quality of life
Virtual ward technologies, such as video consultations and biometric sensors, enable constant patient monitoring, thus, reducing the need for physical examinations and hospital admissions while ensuring care is provided in the comfort of the patient’s home. This approach is especially beneficial for older individuals and those patients with chronic conditions, offering them an opportunity for enhanced quality of life based on independence and autonomy. Families of patients also experience peace of mind, knowing their loved ones are safe and receiving appropriate care.
Additionally, the sense of being actively involved in their own care promotes patient satisfaction and awareness of their condition and support needs.1
Healthcare Providers internationally start to provide home hospital care
There is a growing adoption of home hospital technologies by national healthcare providers. For instance, the NHS in the UK has made a significant commitment to Virtual Wards, with the goal of treating up to 50,000 patients per month and enhancing cost-effectiveness and healthcare outcomes 4.
Additionally, countries like Australia have placed their trust in Virtual Wards, as evidenced during the Covid-19 Omicron Wave. In this period, over 7,000 COVID-19 patients were successfully monitored through virtual wards, resulting in minimal hospitalizations 5. These examples showcase the potential and effectiveness of Virtual Wards in revolutionizing healthcare delivery and improving patient care.
Conclusions
Virtual wards represent a groundbreaking approach to healthcare delivery, revolutionizing the way patients receive care, reducing waiting lists and reducing the strain on hospital staff. By leveraging healthcare monitoring technology and remote patient monitoring, virtual wards offer a viable solution for various patient cohorts, including the elderly, frail, and respiratory patients.
Virtual wards not only reduce hospital readmissions but also optimize costs, increase bed capacity, and provide patients with the comfort and familiarity of their own homes. As the healthcare system continues to evolve, virtual wards have the potential to transform the way we think about healthcare delivery, creating a brighter future for patients, providers, and healthcare systems worldwide.
BlueEye Virtual Ward is an integrated turnkey platform from RedZinc, consisting of wearable sensors, video technology and software platform to monitor and deliver care to the patients at home.
Contact us today at support@blueeye.video to discuss your BlueEye virtual ward.
Follow RedZinc on Twitter and LinkedIn
Sources
1- Chief Nursing Officer’s Office, Department of Health & Office of the Nursing and Midwifery Directorate, Health Service Executive. (2021). The testing and results of an integrated nurse-led community virtual ward proof-of-concept. Office of the Chief Nurse. https://assets.gov.ie/138959/f389d9a6-2a32-4c57-aa8d-98f9aa9c8de4.pdf
2- Lewis, C., Moore, Z., Doyle, F., Martin, A., Patton, D., Nugent, L.E. (2017). A community virtual ward model to support older persons with complex health care and social care needs. Clin Interv Aging. 2017; 12: 985–993 [online]. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5498784/
3- Lewis, C., O’Caoimh, R., Moore, Z., O’Connor, T., Patton, D., Nugent, L.E (2020). Risk Prediction for Adverse Outcomes for Frail Older Persons with Complex Healthcare and Social Care Needs Admitted to a Community Virtual Ward Model. Clin Interv Aging. 2020; 15: 915–926 [online]. online 2020 Jun 22. doi: 10.2147/CIA.S236895
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7320026/
4- Realising the potential of virtual wards. (2023, May 23). NHS Confederation.
https://www.nhsconfed.org/publications/realising-potential-virtual-wards
5- News-Medical.net. (2023, May 16). Outcomes from an Australian COVID-19 virtual ward during Omicron wave. https://www.news-medical.net/news/20221108/Outcomes-from-an-Australian-COVID-19-virtual-ward-during-Omicron-wave.aspx